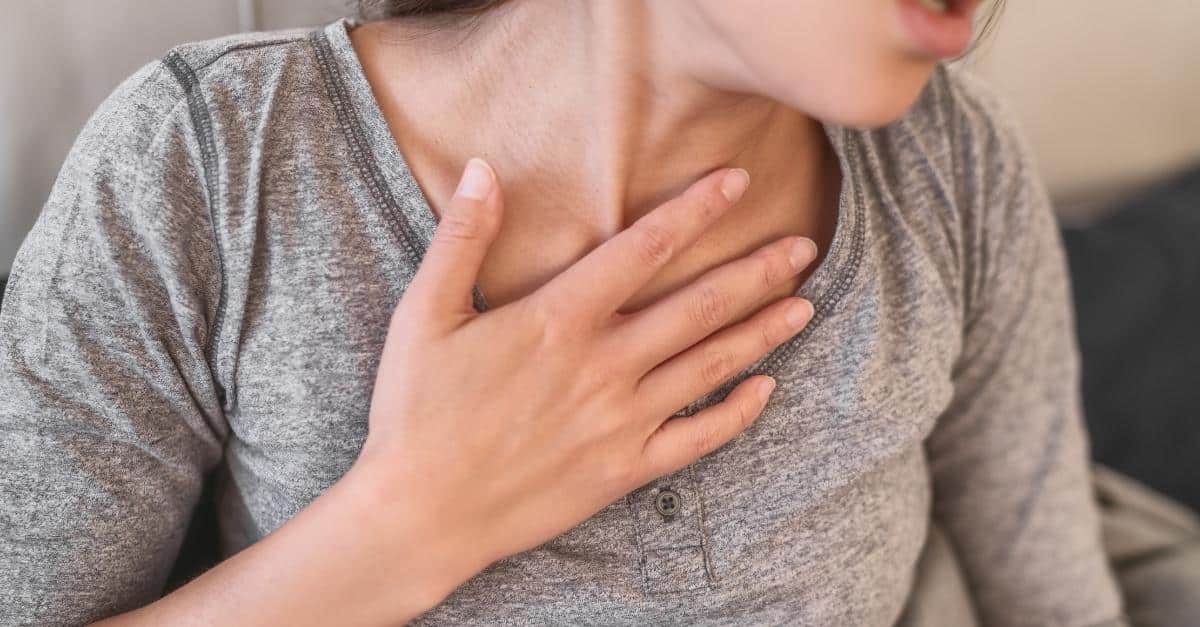
People living with chronic lung diseases often experience breathing difficulties or shortness of breath.
Most people feel that shortness of breath is one of the most concerning symptoms of chronic lung diseases.
Chronic lung diseases make it difficult for people to breathe normally, so people often have trouble maintaining adequate blood oxygen levels.
The respiratory system brings oxygen into the body and delivers it to the body. The soft, spongy lungs don’t have any muscles within them, so they need surrounding muscles and bones to help them work.
During shortness of breath, it can feel as though you cannot breathe normally.
We’re here to help with the information you need about breathlessness and the best positions to reduce shortness of breath.
Experiencing Breathing Difficulties? Use These Positions To Reduce Shortness of Breath.
In combination with the pursed lips breathing and the diaphragmatic breathing techniques, these positions to reduce feelings of shortness of breath can help you relax and reduce the sensation of breathlessness.
Sitting Positions to Reduce Breathing Difficulties:
Typically, shortness of breath happens during physical activity, emotional experiences, bad or changing weather conditions, or when you feel tense or stressed.
Try these sitting positions to reduce shortness of breath:
Sitting Position A:

- Sit in a chair or in a comfortable position
- Keep your feet flat on the floor
- Lean your chest forward a little
- Rest your elbows on your knees
- Place your chin in your hands (if you feel comfortable doing so)
- Relax your neck and shoulders as much as you can
- Practice your breathing techniques
Sitting Position B:

- If a pillow is easily available, place it on a table
- Sit in a chair at the table
- Keep your feet flat on the floor
- Lean your chest forward some
- Place your arms on the table
- Relax your head on your forearms (if a pillow isn’t available) or rest your head on the pillow
- Use your breathing techniques
Standing Positions to Reduce Breathing Difficulties:
Sometimes, shortness of breath happens suddenly. If a chair or a place to do the sitting positions isn’t available, give a standing position to reduce shortness of breath a try:
Standing Position A:
- Find a sturdy wall
- Stand with your feet shoulder-width apart
- Lean your hips on the wall
- Let your hands rest on your thighs
- Allow your shoulders to relax
- Lean forward slightly
- Let your arms dangle in front of you
- Remember to practice your breathing techniques
Standing Position B:
- Find a strong piece of furniture (just below shoulder height), such as a table
- Stand at the furniture
- Place your elbows or hands on the chosen furniture
- Lean forward a little
- Relax your neck and shoulders
- You can rest your head on your forearms if your elbows are on the furniture
- Utilize your breathing techniques
Sleeping Positions to Reduce Breathing Difficulties:
If you’re at home or are awakened by an episode of shortness of breath, remain calm and consider these sleeping positions to reduce shortness of breath:
Sleeping Position A:
- Lie on your side
- Place a pillow between your knees
- Elevate your head with a pillow or two
- Keep your back as straight as possible
- Relax and use your breathing techniques

Sleeping Position B:
- Lie on your back
- Place a pillow under your knees so your knees are bent
- Elevate your head with a pillow or two
- Allow yourself to relax
- Practice your breathing techniques
FAQs
- Is it easier to breathe lying down or sitting up?Generally, you can breathe easier while sitting. The best sitting position is when your hips are above your knees, and they are at their highest point on the floor without putting your feet on the ground. When you are sitting in this position, your lung vital capacity increases and makes it easier to breathe. It’s also easier for the lungs to clear out excess fluid when they’re in an upright position, which is why people will notice that shortness symptoms are relieved once they stop lying down.
- Why does leaning forward help breathing?If you bend forward at the waist, you may notice that breathing becomes easier. This position can reduce shortness of breath while you are both exercising or resting. Bending forward may help with breathing difficulties because the diaphragm moves more easily. As you may or may not know, your diaphragm is a large muscle between your lungs and your belly. It works to draw air into your lungs as you breathe and being in a better position enables your diaphragm to work more efficiently.
- What muscles are used for breathing?To better understand the shortness of breath, it’s important to know about the muscles used for breathing. Breathing can be a voluntary or involuntary act. For example, you can voluntarily hold your breath or take a slow, deep breath. Involuntary breathing occurs when you breathe without thinking about breathing at all, such as when you sleep. Because the lungs themselves don’t contain any muscles, they need help from muscles within the body. The intercostal muscles are small and numerous muscles situated between each rib and on each side of each rib. The intercostal muscles help enlarge the chest cavity and contract to pull the ribcage both upward and outward as you inhale. The diaphragm is the most important muscle for breathing. In fact, the diaphragm has its own nerve supply and can work involuntarily and voluntarily. The diaphragm works like a vacuum. When the diaphragm contracts during inhalation, it goes down toward the stomach, expands the lungs, and pulls new air into them. During exhalation, the diaphragm relaxes and moves back to its original position. As the diaphragm relaxes, it and the intercostal muscles in the ribcage push old air back out of the lungs. The intercostal muscles also relax and reduce the space in the chest cavity.
Accessory Muscles
If you are under stress, have an injury, or are experiencing difficulty breathing, accessory muscles can help you breathe. Accessory muscles are not used during normal breathing. The accessory muscles sometimes used for breathing include the muscles in front of the neck, the chest pectorals, and the abdominal muscles. For people with chronic obstructive pulmonary disease (COPD), the air becomes trapped in the lungs, making it harder for them to expel air. Many people with chronic lung diseases use accessory muscles to help them breathe in and out. - What is shortness of breath?Shortness of breath is a common and often frightening symptom of chronic lung diseases. Many people describe breathlessness as air hunger. Shortness of breath makes people feel unable to fill their lungs with oxygen. Sometimes, shortness of breath happens suddenly and without a known cause. It often occurs with chest tightness and anxiety and is a common symptom of COPD Exacerbation. If you experience shortness of breath, follow your doctor’s instructions and use prescribed inhalers as directed by your doctor. While frightening, remember to stay calm and consider trying the following positions to reduce shortness of breath.
Taking Steps Toward Easier Breathing
Following your doctor’s advice, taking your medications properly, and learning about all of your treatment options help you stay proactive in your healthcare.
In combination with your current treatment plan and breathing techniques, we hope these positions to reduce shortness of breath help you stay calm and breathe easier.

Christine Kingsley, APRN is the Health and Wellness Director at the Lung Institute where she focuses on providing helpful online resources for people looking for information on various lung diseases, breathing exercises, and healthy lifestyle choices. She advocates for holistic care that involves working with your doctor to explore all options including traditional and alternative care while focusing on diet and exercise as proactive measures.