People living with chronic lung diseases, such as chronic obstructive pulmonary disease (COPD), emphysema and pulmonary fibrosis, often have lung function tests.
Sometimes, lung function tests are called pulmonary function tests (PFTs), and doctors use these lung function tests to diagnose chronic lung diseases, assess how well your lungs work as well as to monitor how well your treatment plan works.
Lung function tests can measure lung size, airflow, how well gases move in and out of your blood and more. To help you better understand lung function tests, we’ve put together this complete guide with the information you need.
Lung Function Tests:
There are several types of lung function tests. A single type of lung function test cannot determine all of the lung function values, so more than one type of lung function test may be needed.
In addition, some of the tests may be repeated after you inhale a bronchodilator to open your airways. Now, your doctor can compare your test results with and without medication, and it will help your doctor develop an individualized treatment plan.
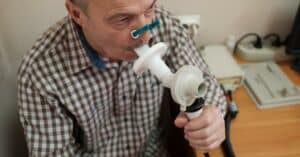
Spirometry Tests
During spirometry, you breathe into a tube attached to a machine called a spirometer. Spirometry measures your airflow. These measurements include how much air you inhale and exhale as well as how quickly you can exhale.
Forced vital capacity (FVC) and forced expiratory volume in one second (FEV1) are two important measurements gained from spirometry.
FEV1 and FVC results give doctors valuable information about how your lungs work. FVC is the total amount of air you can breathe out after taking the deepest breath possible.
FEV1 is the amount of air you can forcefully exhale during the first second of the FVC test.
Body Plethysmography Tests
Body plethysmography measures how much air is in your lungs after taking a deep breath. It also measures how much air remains in your lungs after you exhale as much as possible.
Total lung capacity (TLC) is the total amount of air your lungs can hold, and residual volume (RV) is the amount of air still in your lungs after you exhale as much as you can.
Body plethysmography shows your doctor how well your lungs function. Like spirometry, your doctor may perform multiple body plethysmography tests to compare results, to measure the progression of your chronic lung disease and to develop or modify your treatment plan.
During body plethysmography, you sit in an enclosed, clear box that looks like a telephone booth. Then, you will wear a nose clip and breathe into the mouthpiece while measurements are recorded.
Gas Diffusion Tests
Gas diffusion tests show doctors the amount of oxygen and other gases that move through the lungs’ tiny air sacs (alveoli). These types of lung function tests measure how well gases, such as oxygen, are being absorbed into your blood from your lungs.
Two common types of gas diffusion tests include the arterial blood gas test and the carbon monoxide diffusion capacity test (DLCO).
The arterial blood gas test (ABG) measures the amount of oxygen and carbon dioxide in your blood. ABG shows how well your lungs bring oxygen to the bloodstream and remove carbon dioxide from your bloodstream. For the ABG test, blood is drawn from an artery.
The DLCO test shows how well your lungs transfer a small amount of carbon monoxide (CO) into the blood. DLCO measurements are taken after you breathe a very small amount of carbon monoxide. The measurements are either taken while you inhale or as you exhale.
Exercise Tolerance Tests
Exercise tolerance tests provide your doctor with valuable information about your exercise capacity. Many people with chronic lung diseases experience shortness of breath, especially during exercise.
However, exercise has been shown to improve quality of life, strength and stamina in many people with lung disease. Understanding how exercise affects your lungs helps doctors develop a well-rounded treatment plan.
The 6-minute walk test measures the distance you can walk on a flat, hard surface in six minutes. Doctors use the 6-minute walk test to understand your ability to perform daily physical activities.
Cardiopulmonary exercise tests evaluate your exercise capacity and are especially useful in assessing decreased exercise capacity and causes of shortness of breath. During cardiopulmonary exercise tests, you walk on a treadmill or ride a stationary bicycle while your heart and lung functions are monitored.
In general, your heart and lungs are watched while at rest, during warm-up, during a short exercise period and during the recovery phase.
Pulse Oximetry Tests
Pulse oximetry tests measure your oxygen saturation level in your blood. The test is simple and painless. In general, a finger-clip type device is placed over your finger or on your earlobe. The light inside the device measures the amount of oxygen in your blood.
Often, people with chronic lung diseases have trouble maintaining an adequate blood oxygen level. Your doctor will use the information gathered from pulse oximetry to make sure you’re receiving enough oxygen.
If your blood oxygen level is too low, your doctor may prescribe oxygen therapy. Oxygen therapy can help improve your blood oxygen level.
How Do You Prepare for Lung Function Tests?
While lung function tests are considered safe, before having the test, it’s important to tell your doctor if you have had recent chest pains or a heart attack, take medicine for a lung condition, are allergic to any medicines, have a collapsed lung and if you had recent surgery on your eyes, chest or belly.
Typically, people are advised not to eat a heavy meal before the test, smoke or perform intense exercise for 6 hours before the test. In addition, people are asked to wear loose fitting clothing. Ask your doctor or nurse to explain the test to you and how to prepare for it.
Following-Up and Taking Care of You
Your doctor will go over your lung function test results with you. Over time, your doctor may recommend repeating lung function tests, so your doctor can accurately monitor your lung function and lung health.
Lung function tests are especially important for people living with chronic lung diseases. You and your doctor will work together to develop the best treatment plan for you.
In general, your treatment plan may include medications, inhalers, pulmonary rehabilitation, oxygen therapy and lifestyle changes. These types of treatments work to help people breathe better and manage lung disease symptoms.
Always consult with your doctor to find a treatment plant that works best for you.

Christine Kingsley, APRN is the Health and Wellness Director at the Lung Institute where she focuses on providing helpful online resources for people looking for information on various lung diseases, breathing exercises, and healthy lifestyle choices. She advocates for holistic care that involves working with your doctor to explore all options including traditional and alternative care while focusing on diet and exercise as proactive measures.