Pulmonary function tests (PFTs) measure how well you breathe. Spirometry is a type of pulmonary function test.
People with chronic lung diseases often have pulmonary function tests, including spirometry.
We’re here to give you the information you need about spirometry, how it works and why it’s important.
What is Spirometry?
Simply put, spirometry measures your airflow. Doctors use spirometry to test how well your lungs work. Spirometry tests measure how much air you inhale, how much air you exhale and how quickly you exhale.
Two important measurements gained from the test include FEV1 and FVC results.
Measurements Determined with Spirometry Include:
- Forced Vital Capacity (FVC)—The total amount of air you can breathe out after taking the deepest breath possible.
- Forced Expiratory Volume in One Second (FEV1)—The amount of air you can forcefully exhale during the first second of the FVC test.
- Peak Expiratory Flow Rate (PEFR)—PEFR measures how fast a person can breathe out, and the estimated value depends on gender, ethnicity, height, weight and age.
- Total Lung Capacity (TLC)—The total amount of air in the lungs after a deep inhalation.
- Forced Expiratory Volume (FEV)—The amount of air forcefully blown out of the lungs during the first, second and third seconds of the FVC test.
- Maximum Voluntary Ventilation (MVV)—The amount of air a person can breathe in and out in one minute.
- Forced Expiratory Flow (FEF)—The flow or volume in the middle of an exhalation.
- Functional Residual Capacity (FRC)—The amount of air that stays in the lungs after a normal breath.
- Tidal Volume (VT)—The amount of air inhaled or exhaled while breathing normally.
- Minute Volume (MV)—The amount of air exhaled per minute.
- Vital Capacity (VC)—The total volume of air you can exhale after inhaling as much as possible.
Why is Spirometry Used?
Spirometry is used to diagnose chronic lung diseases, such as chronic obstructive pulmonary disease (COPD) and emphysema.
Some doctors also use spirometry to monitor your current treatment plan. If you’re doctor finds that your treatment isn’t working well, he or she may decide to try another course of treatment.
What Happens during a Spirometry Test?
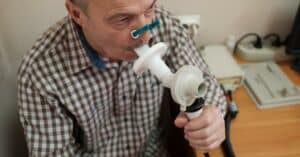
During a spirometry test, you breathe into a tube that attaches to a machine. The machine is called a spirometer.
The doctor, nurse, respiratory therapist or medical professional performing the test will give you instructions. Listen to the instructions and ask questions if something is unclear.
For the most accurate results, it’s important to understand what you’re expected to do and to do the test correctly.
Generally, you can expect the following:
- You will likely be sitting.
- To keep your nostrils closed, a clip will be placed on your nose.
- You will be asked to create a seal around the tube with your lips.
- Some of the test measurements include breathing normally.
- You will take a deep breath, and then breathe out as hard as you can for several seconds into the tube.
- You will likely repeat the test three times to ensure consistent results.
- If your results vary too much, you may have to repeat the test.
- Typically, the highest value of three close test results is used as the final result.
- The entire process takes around 15 minutes to complete but may take longer.
Sometimes, your doctor may give you a bronchodilator inhaler after your initial spirometry tests. A bronchodilator inhaler works to open your airways. Typically, you will wait 15 minutes before doing another round of testing.
Your doctor will compare your initial spirometry results to your spirometry results after using a bronchodilator. Comparing these results helps your doctor know if a bronchodilator has improved your airflow.
What is the Importance of Spirometry?
For people with chronic lung diseases, having lung function testing is highly important. In addition to lung function measurements, spirometry indicates whether or not there is airway obstruction or airway restriction.
It helps doctors diagnose different types of chronic lung diseases, such as obstructive and restrictive lung diseases.
Lung function and pulmonary function test results differ for obstructive and restrictive lung diseases.
In fact, spirometry helps your doctor understand how well your lungs and treatment plan are working. Chronic lung diseases are progressive conditions and will worsen over time.
It’s important to monitor your lungs, keep track of how well your treatment plan is working and the progression of the condition. Treatments could include inhalers, corticosteroids, oxygen therapy, diet and exercise.

Christine Kingsley, APRN is the Health and Wellness Director at the Lung Institute where she focuses on providing helpful online resources for people looking for information on various lung diseases, breathing exercises, and healthy lifestyle choices. She advocates for holistic care that involves working with your doctor to explore all options including traditional and alternative care while focusing on diet and exercise as proactive measures.