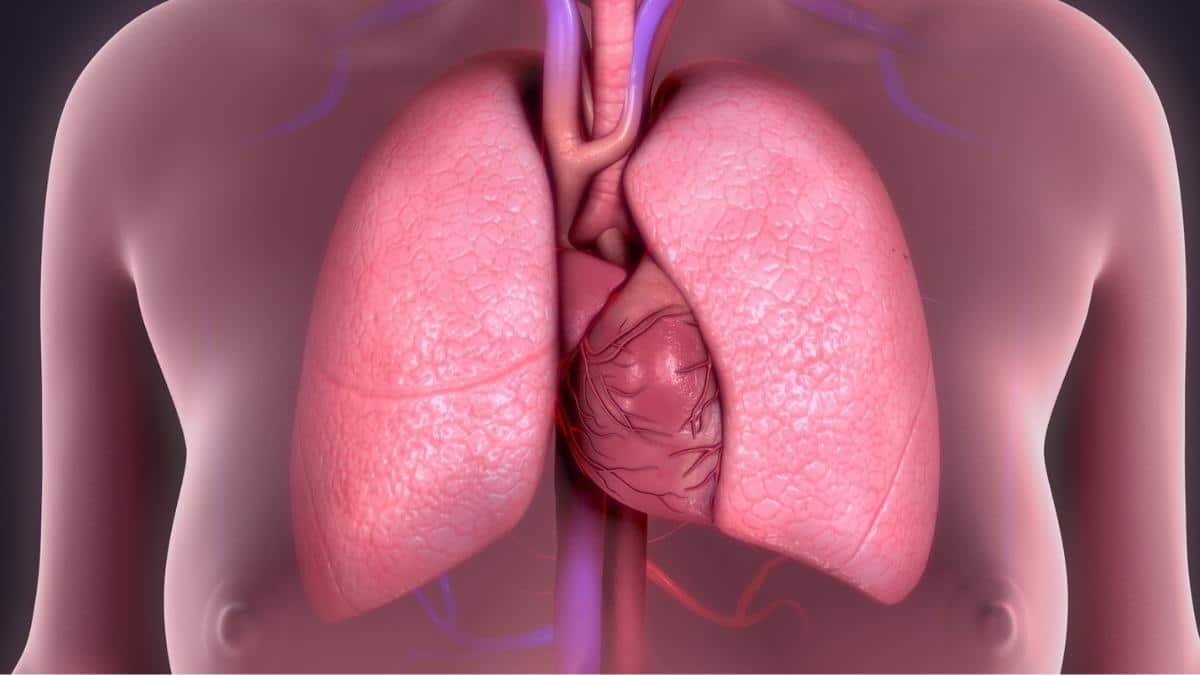
The number one cause of death in the United States is heart disease, and the second leading is cancer. However, what many people might not know is that the third leading cause of death is chronic lower respiratory diseases, such as chronic obstructive pulmonary disease (COPD).
COPD and heart problems, specifically heart failure, have one serious symptom in common—difficulty breathing. Often, people with COPD and people with heart failure have difficulty exercising, walking distances and climbing stairs.
If you have COPD and heart problems, it can be difficult to pinpoint which disease is causing your shortness of breath. In some instances, it could be a combination. Here’s what you need to know about the relationship between COPD and heart problems.

Shortness of Breath: Heart Failure or COPD?
COPD and heart problems are complex conditions that can cause shortness of breath. It’s important to know the differences in shortness of breath with COPD and heart failure.
Shortness of Breath Caused by Heart Failure
In patients with heart failure, the heart has difficulty pumping blood. When a person with heart failure is in a resting state, they tend not to have much difficulty breathing. However, under a bit of exertion, the heart must work harder to pump blood to the body and the lungs.
If the heart cannot keep up with the demand for blood throughout the body, blood can back up in the lungs, resulting in fluid congestion and shortness of breath.
Shortness of Breath Caused by COPD
As in cases of heart failure, people with COPD tend to maintain a normal rate of breathing while at rest. However, when an individual with COPD becomes active, the lungs cannot bring in enough oxygen, despite heavy breathing.
When a person with COPD exhales, not all of the oxygen is pushed out of the lungs. Oxygen is trapped in the intricate pathways and damaged tissues of the lungs. As a result, people inhale their next breath before all of their previous breath has been expelled. The result is shortness of breath.
Major Types of Heart Failure
According to the American Heart Association, there are three major types of heart failure: left-sided, right-sided and congestive.
Left-sided Heart Failure
The two major types of left-sided heart failure are systolic and diastolic. Systolic failure occurs when the left ventricle can no longer contract normally. This prevents the heart from pumping with enough force to push blood into circulation.
Diastolic failure happens when the left ventricle loses its ability to relax normally because the heart muscle has become stiff. As a result, the heart cannot properly fill with blood during the resting period between each beat.
Right-sided Heart Failure
Right-sided heart failure usually occurs as a result of some form of left-sided heart failure. When the left ventricle fails, the right ventricle has difficulty performing its job of transferring “used” blood back into the lungs for re-oxygenation.
This results in increased fluid pressure, and weakness in the right ventricle. Often, people with right-sided heart failure experience symptoms such as swelling in the legs, ankles and abdomen because blood backs up in the veins.
Congestive Heart Failure
Congestive heart failure occurs when the blood flow out of the heart slows down. As a result, blood returning to the heart gets backed up in the veins causing congestion throughout the body, including the lungs.
This can result in edema, or swelling of the legs and ankles. Sometimes fluid also collects in the lungs, which is called pulmonary edema.
COPD and Left-Sided Heart Failure
COPD is not directly related to left-sided heart failure, but the two conditions can exacerbate each other. When blood is not properly oxygenated due to COPD, extra stress is placed on the heart, worsening the symptoms of left-sided heart failure.
Conversely, excess fluid in the lungs from left-sided heart failure can make breathing more difficult for someone with COPD. High blood pressure and coronary artery disease often result in left-sided heart failure.
COPD and Right-Sided Heart Failure
During right-sided heart failure, COPD can have a direct influence on the heart’s right ventricle. Pulmonary hypertension results when the blood pressure inside the arteries rises. This can be in response to abnormally low oxygen levels in the vessels inside the lungs as a result of COPD.
The excess strain from pulmonary hypertension on the right ventricle can result in heart failure. Right-sided heart failure causes fluid to accumulate in the legs, ankles and abdomen as well as the lungs. It is important to note that medical conditions other than COPD can also be responsible for right-sided heart failure.
How Do I Know If I Have COPD and Heart Problems?
If you are concerned about COPD and heart problems or if you think you may be experiencing them, it is important to talk to your doctor immediately. Fatal congestive heart failure can strike without warning.
However, multiple types of medication can help control hypertension and other conditions that can lead to heart failure.
If prescription medications fail, surgical procedures can be performed to return heart function. Healthy eating habits, such as a reduced or low sodium diet, eating plenty of fruits and vegetables and consuming lean protein can help you manage symptoms if you have COPD and heart problems as well.
If you have COPD and heart problems, your doctor may ask you to monitor your weight, breathing and appetite to keep track of how you’re doing and how well your treatment is working. If you experience increased swelling in your feet, legs or abdomen, it is important to speak with a doctor.
There are also medications, treatments and alternative options available to people with COPD.
Always consult with your doctor to find a treatment plan that works best for you.

Christine Kingsley, APRN is the Health and Wellness Director at the Lung Institute where she focuses on providing helpful online resources for people looking for information on various lung diseases, breathing exercises, and healthy lifestyle choices. She advocates for holistic care that involves working with your doctor to explore all options including traditional and alternative care while focusing on diet and exercise as proactive measures.