It might sound strange, but the respiratory and digestive systems depend on one another for optimal function.
Because oxygen is essential to the proper functioning of the body, one of the main concerns for people with chronic lung diseases is maintaining enough oxygen in their blood.
The body needs energy and oxygen, so let’s take a closer look at oxygen levels and the digestive system.
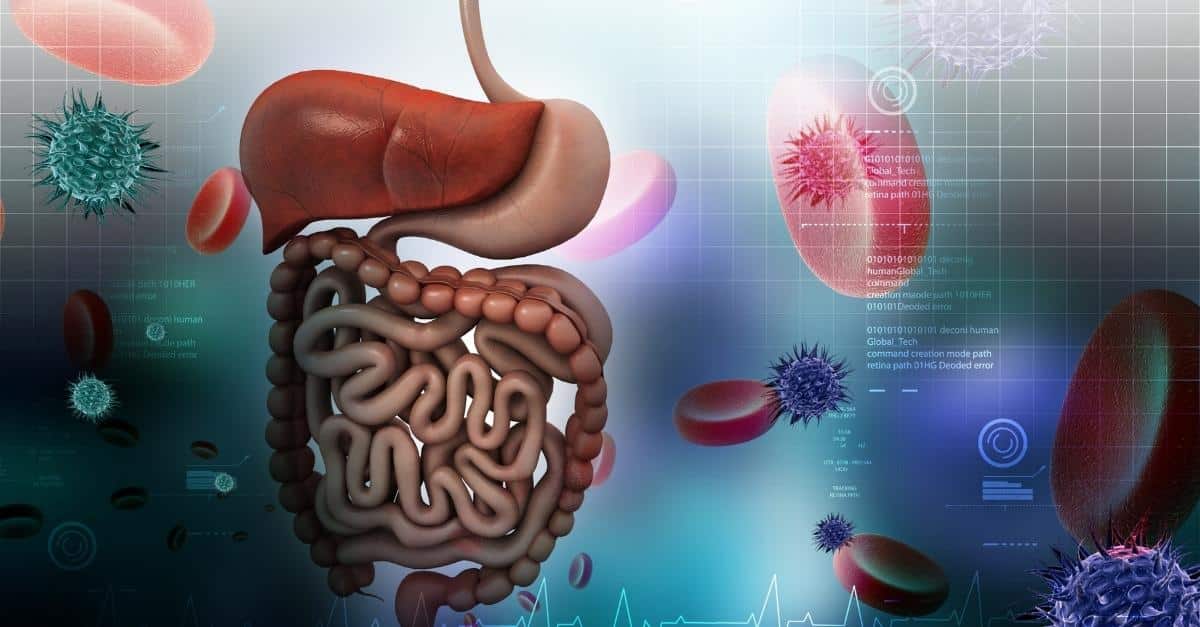
What does the digestive system do?
The digestive system breaks down food so that it can become energy for the body. The digestive system is comprised of a complex system of organs, nerves, hormones, bacteria and blood work together to digest food.
Digestive organs include the stomach, small intestines, large intestines, liver, pancreas and gall bladder.
What’s the connection between the respiratory, oxygen levels, and digestive systems?
The respiratory and digestive systems work together to power the body. A properly functioning respiratory system delivers adequate oxygen to the blood.
Because the digestive system breaks down food and uses muscular contractions to move food through the digestive tract, it needs oxygen to function properly.
In turn, the respiratory system depends on a properly functioning digestive system to provide the fuel it needs to work effectively. Each function of the body depends on other functions, and all parts of the body need fuel and oxygen.
What are the risks of having lung disease and digestive system conditions?
In many cases, oxygen levels and the digestive system go hand-in-hand. COPD and other chronic lung diseases carry a risk for certain digestive disorders. Because some foods and drinks can cause symptom flare-ups, it’s important to know what to eat and what to avoid.
Foods such as dairy and cruciferous vegetables are linked to increased mucus production and gas. Certain foods can also make GERD symptoms worse.
GERD or gastroesophageal reflux disease is common among people with COPD. GERD is a digestive disorder in which the stomach valve that keeps stomach acid down weakens or malfunctions, allowing stomach acid into the esophagus.
If stomach acid reaches the lungs, it can result in irritation, increased coughing, and shortness of breath.
GERD Symptoms include:
- Dry cough
- Chest pain
- Difficulty swallowing
- Hoarseness or sore throat
- Burning in the chest or throat
- The sensation of a lump in the throat
- Regurgitation of stomach contents
What can I do to improve my blood oxygen levels?
Talk with your doctor about any new or worsening symptoms. See your doctor regularly, even if you’re feeling well.
Now that you have information about oxygen levels and the digestive system, discuss your oxygen, food, and exercise needs with your doctor. You and your physician can decide on the best treatment plan for you.

Christine Kingsley, APRN is the Health and Wellness Director at the Lung Institute where she focuses on providing helpful online resources for people looking for information on various lung diseases, breathing exercises, and healthy lifestyle choices. She advocates for holistic care that involves working with your doctor to explore all options including traditional and alternative care while focusing on diet and exercise as proactive measures.