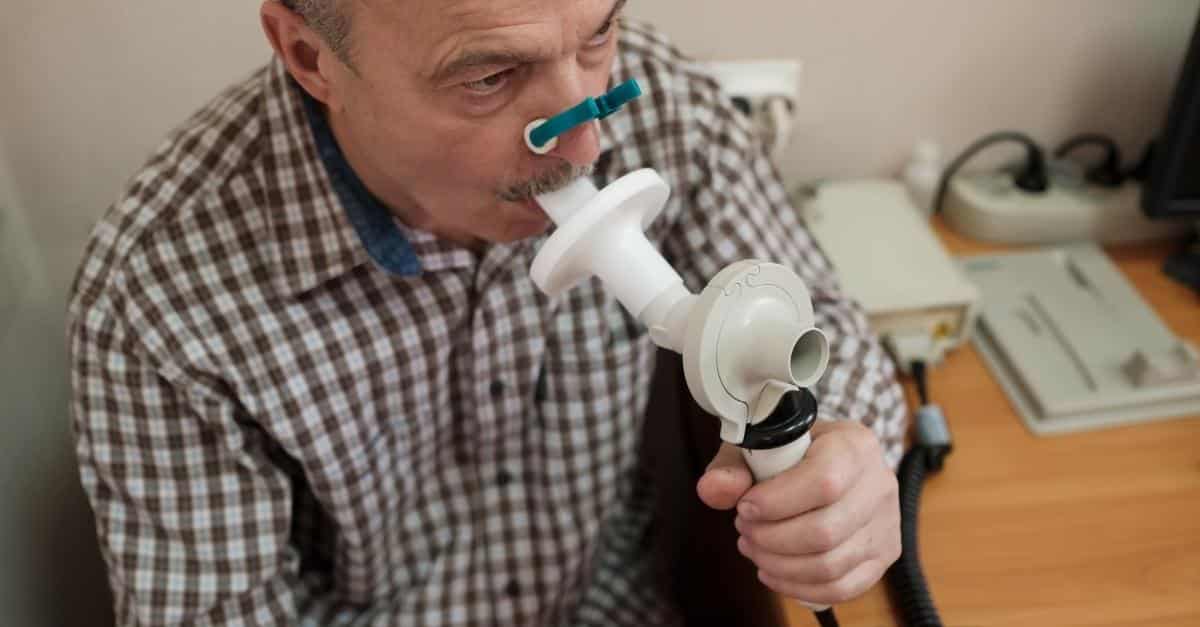
People living with chronic lung diseases, such as chronic obstructive pulmonary disease (COPD), emphysema and pulmonary fibrosis, often have their pulmonary function tested.
Many doctors use lung function tests to help diagnose, monitor, and treat chronic lung diseases. Lung function tests are also referred to as pulmonary function tests (PFTs).
Two important measurements gained from pulmonary function tests are forced expiratory volume in one second (FEV1) and forced vital capacity (FVC).
To help you better understand FEV1 and FVC, we’ve put together the important facts about what these measurements mean for you.
How are FEV1 and FVC Measured?
Forced expiratory volume in one second (FEV1) and forced vital capacity (FVC) are measured during a pulmonary function test.
A diagnostic device called a spirometer measures the amount of air you inhale and exhale, and the amount of time it takes for you to exhale completely after a deep breath.
The spirometer attaches to a machine that records your lung function measurements for pulmonary function tests.
What is FVC?
The forced vital capacity (FVC) measurement shows the amount of air a person can forcefully and quickly exhale after taking a deep breath.
Determining your FVC helps your doctor diagnose chronic lung disease, monitor the disease over time, and understand the severity of the condition.
In general, doctors compare your FVC measurement with the predicted FVC based on your age, height, and weight.
What is FEV1?
Forced expiratory volume is measured during the forced vital capacity test.
The forced expiratory volume in one second (FEV1) measurement shows the amount of air a person can forcefully exhale in one second of the FVC test.
In addition, doctors can measure forced expiratory volume during the second and third seconds of the FVC test.
Determining your FEV1 measurement helps your doctor understand the severity of the disease. Typically, lower FEV1 scores show more severe stages of lung disease.
FEV1 and FVC are related and followed closely.
FEV1 and FVC Ratio
FVC can decrease in a similar way in both obstructive lung diseases (COPD) and restrictive lung diseases (pulmonary fibrosis).
Often, doctors use the FVC and FEV1 ratios to figure out the specific type of lung disease.
For example, when FEV1 values make up less than 80% of the FVC, an obstructive lung disease is likely present. However, in restrictive lung diseases, both the FEV1 and FVC measurements decrease proportionally.
To determine the FEV1 and FVC ratio, your doctor will divide your FEV1 into your FVC.
What Chronic Lung Diseases Are Associated with a Decreased FVC?
Chronic lung diseases affect everyone differently and progress at different rates.
Your doctor may perform additional pulmonary function tests to monitor your FEV1 and FVC as well as other lung function measurements.
Chronic lung diseases associated with a decreased FVC include:
- COPD
- Emphysema
- Chronic Bronchitis
- Pulmonary Fibrosis
- Inflammatory Lung Diseases
- Other Restrictive and Obstructive Airway Diseases
What Steps Can You Take?
Knowing your FEV1 and FVC will help you and your doctor understand the severity of your lung disease. You and your doctor will work together on a treatment plan.
Remember to see your doctor regularly, even if you are feeling well. Your doctor will monitor your lung disease symptoms, lung health, and overall health to ensure your treatment plan is working well for you.
Call your doctor if you see changes in your lung health or symptoms.
In addition to their typical treatment plan, some patients have tried lifestyle changes and alternative therapies.
For example, eating a healthy diet and exercising can help with certain lung disease symptoms, such as shortness of breath.
Cellular therapy has helped some people return to their favorite activities.

Christine Kingsley, APRN is the Health and Wellness Director at the Lung Institute where she focuses on providing helpful online resources for people looking for information on various lung diseases, breathing exercises, and healthy lifestyle choices. She advocates for holistic care that involves working with your doctor to explore all options including traditional and alternative care while focusing on diet and exercise as proactive measures.